What is Continuous Glucose Monitoring (CGM)?
Continuous Glucose Monitoring (CGM) devices are innovative tools designed to assist individuals in managing diabetes more effectively, reducing the reliance on frequent fingerstick tests. These systems utilize a sensor placed just beneath the skin to continuously monitor glucose levels throughout the day and night. The collected data is transmitted to a wearable device or smartphone, allowing users to track glucose fluctuations in real-time. While becoming proficient with CGM technology requires an initial learning period, it offers a significant advancement in personalized health management.
Overview
CGM systems provide various options for displaying glucose data, including integration with insulin pumps, smartwatches, smartphones, or dedicated handheld devices.
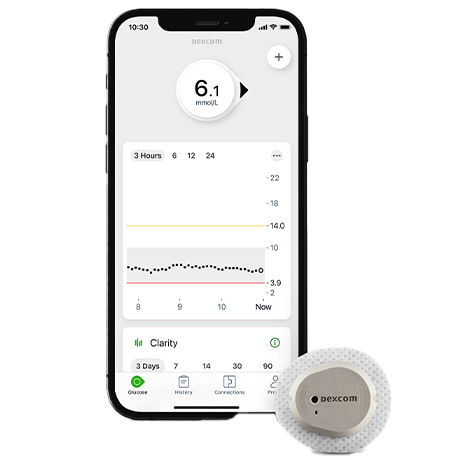
Understanding Continuous Glucose Monitoring (CGM)
CGM represents a leap forward in wearable health technology, offering continuous tracking of glucose (sugar) levels. By measuring glucose in the interstitial fluid just beneath the skin, CGMs provide 24/7 monitoring for users. This technology is particularly beneficial for individuals with diabetes, as managing blood sugar levels is crucial to their health. CGMs deliver real-time insights into glucose trends, which is essential given the myriad factors that can unpredictably influence blood sugar levels.
The market offers a variety of CGM devices, with technology advancing rapidly. Some models can connect with insulin pumps to facilitate automated insulin delivery systems. Consulting with a healthcare provider can help determine the most suitable CGM options based on individual health needs.
Consulting Healthcare Providers about CGM
Before integrating a CGM into your health regimen, discuss with your healthcare provider to determine its suitability for your specific needs. They can provide guidance on device selection, usage training, and how to interpret the data effectively.
Common Questions
What is the role of interstitial fluid?
Interstitial fluid surrounds the body’s cells, originating from substances that leak out of blood capillaries, including glucose. CGM sensors are positioned just under the skin within this fluid, rather than directly in blood vessels, to measure glucose levels.
It’s important to note that glucose first enters the bloodstream before diffusing into the interstitial fluid. Consequently, CGM readings may exhibit a slight delay compared to direct blood glucose measurements, typically by a few minutes.
How do CGM Devices Operate?
Despite the variety of CGM devices available, they generally consist of three primary components:
- Sensor: A small device inserted under the skin, usually on the abdomen or arm, using an applicator. The sensor measures glucose levels in the interstitial fluid and typically remains in place for 7 to 15 days, depending on the brand. Some implantable sensors have a longer lifespan and are inserted by a healthcare professional.
- Transmitter: This component wirelessly sends glucose data from the sensor to a display device. In some systems, the transmitter is reusable and attaches to each new sensor; in others, it’s integrated into the disposable sensor.
- Display Device: This could be a smartphone app, a dedicated receiver, or an insulin pump that shows current glucose levels, historical data, and trends. Many CGMs offer customizable alerts for glucose levels that are too high or too low.
What is the general operation process?
- Sensor Insertion: The user places a small sensor under the skin using an applicator. Adhesive patches secure the sensor in place.
- Transmitter Attachment: Depending on the system, the transmitter is either attached to the sensor or is already integrated. Some transmitters require charging before use. Additional adhesive may be applied to ensure the assembly remains secure.
- Initialization Period: After insertion, the sensor may require a warm-up period, typically ranging from 30 minutes to two hours, before it begins transmitting data.
- Calibration: Certain CGM models require calibration with traditional fingerstick blood glucose readings to maintain accuracy.
- Monitoring: Once operational, the system provides continuous glucose readings to the display device. Users can set personalized alerts for glucose levels that fall outside their target range.
- Sensor Replacement: After the sensor’s designated lifespan ends, the user replaces it by repeating the insertion process.
CGM data can be downloaded for long-term analysis and shared with healthcare providers to inform treatment decisions.
How easy is it to use a CGM?
While CGMs are sophisticated devices, learning to use them effectively involves:
- Proper Sensor Insertion: Ensuring accurate placement for reliable readings.
- Device Calibration: If required, calibrating the CGM with fingerstick tests.
- Setting Alerts: Customizing alarms for high or low glucose levels.
- Data Management: Downloading and interpreting glucose data to identify patterns and trends.
Training is often provided to help users become proficient with their CGM devices, ensuring they can maximize the benefits of continuous glucose monitoring.
Do CGMs Eliminate the Need for Fingerstick Tests?
While CGMs significantly reduce the frequency of fingerstick tests, it’s advisable to keep a traditional glucose meter available to:
- Confirm CGM Readings: Especially if symptoms don’t align with sensor data.
- Calibrate the Device: For models that require periodic calibration to maintain accuracy.
- Serve as a Backup: In case of device malfunctions or sensor issues, ensuring continuous glucose monitoring.
Can Individuals Without Diabetes Benefit from CGMs?
While CGMs are primarily designed for those with diabetes, they may also be beneficial for individuals with conditions affecting glucose levels, such as:
- Prediabetes
- Obesity
- Certain Metabolic Disorders
- Insulinoma
Consulting a healthcare provider can help determine if CGM technology is appropriate for your specific health situation.
What are some advantages to Using a Continuous Glucose Monitor (CGM)
Continuous Glucose Monitors (CGMs) offer a range of benefits that enhance diabetes management and overall health monitoring:
- Comprehensive Glucose Profiling: CGMs provide continuous tracking of glucose levels, offering a detailed view of fluctuations throughout the day and night. This real-time data enables users to observe trends and make informed decisions about their health.
- Proactive Health Management: By delivering immediate alerts for glucose levels that are too high or too low, CGMs empower users to take swift corrective actions, potentially preventing severe hypoglycemic or hyperglycemic episodes.
- Enhanced Personalization: The detailed data from CGMs allows for tailored adjustments in diet, physical activity, and medication. This personalized approach can lead to improved glycemic control and a reduction in HbA1c levels.
- Reduced Need for Fingerstick Tests: With continuous monitoring, the dependence on traditional fingerstick tests decreases, making diabetes management less intrusive and more convenient.
- Data Sharing Capabilities: Many CGM systems offer features that allow users to share their glucose data with healthcare providers and family members, facilitating collaborative care and support.
What are some considerations and limitations to using a CGM?
While CGMs present numerous advantages, it’s essential to be aware of certain considerations:
- Accuracy Variations: Factors such as rapid glucose changes, medication interference, or device calibration issues can affect CGM accuracy. It’s advisable to confirm unusual readings with a traditional blood glucose meter.
- Lag Time: CGMs measure glucose in interstitial fluid, which may lag behind blood glucose levels by several minutes. This delay is generally minimal but can be significant during rapid glucose fluctuations.
- Cost and Insurance Coverage: The expense of CGM devices and supplies can be considerable, and insurance coverage varies. It’s important to verify benefits with your insurance provider.
- Physical Considerations: Wearing a CGM involves having a device attached to the body, which may cause discomfort or skin irritation for some users.
